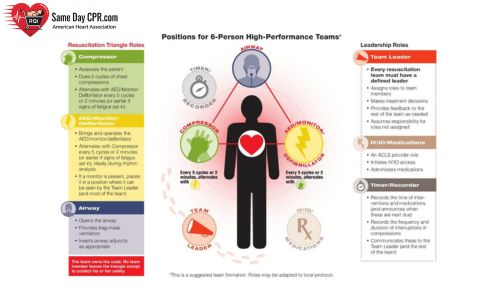
In a cardiac emergency, teamwork can make all the difference. A high-performance resuscitation team in ACLS (Advanced Cardiovascular Life Support) is a group that works smoothly as one unit. Its goal is to act quickly, share clear goals, and support one another so that every action is coordinated and effective. When roles are well defined, such as the compressor, AED/monitor/defibrillator operator, airway opener, team leader, IV/IO/medications provider, and timer/recorder in a high performance resuscitation team, and everyone knows the plan, the team can communicate fast, stay calm, and adapt to changes in the patient’s condition. This smooth cooperation helps the team stay focused on the patient, reduces delays, and makes the rescue more reliable. There are altogether 6 people in this resuscitation team. The result is better teamwork, faster decisions, and a stronger chance for a positive outcome for the patient. Whether you’re an emergency physician, ACLS instructor, critical care team, or EMS clinician, these roles are suitable for you.
Core Principles of High-Performance Teamwork
In a high-stakes code, teamwork makes all the difference. Understanding each person’s role, staying aware of what’s happening, and communicating helps the team act quickly and confidently.
- Everyone on the team thinks about the same plan and knows what the goals are, so actions stay coordinated.
- Team members speak, confirm messages, and repeat important information to avoid mistakes.
- Each person knows their job, but can step in where needed when the situation changes.
- The team keeps an eye on the patient, the environment, and each other to catch changes quickly.
The Resuscitation Triangle Role
In an ACLS high-performance team, the resuscitation triangle helps everyone know their role during a code. One person leads and gives clear instructions, another focuses on chest compressions and airway, and a third handles medications and monitors the heart rhythm. When each team member knows exactly what to do, care flows smoothly, mistakes are fewer, and the patient gets the best chance to recover.
1. Compressor
The compressor plays a key role in the resuscitation triangle. They check the patient, give five cycles of chest compressions, and keep a steady rhythm. After two minutes or five cycles, they switch with the person handling the AED, monitor, or defibrillator, or swap sooner if they feel tired. This keeps compressions strong and consistent, giving the patient the best chance to recover. For more on how the compressor maintains optimal depth and rate, see the chest compression feedback device for effective CPR.
2. AED/Monitor/Defibrillator
The AED, monitor, or defibrillator person brings and uses the device to check the patient’s heart rhythm and deliver shocks if needed. They switch with the compressor every two minutes or five cycles, or sooner if someone is tired, usually while the rhythm is being analyzed. If a monitor is available, they make sure it is placed where the team leader and everyone else can see it.
3. Airway
The airway person keeps the patient’s airway open and helps them breathe. They use a bag-mask to give breaths and add airway tools when needed. Their work makes sure oxygen reaches the lungs and supports the team’s resuscitation efforts.
Note: The team owns the code. No team member leaves the triangle except to protect his or her safety.
The Leadership Roles
In an ACLS team, leaders guide the group and keep everyone focused. They make quick decisions, assign tasks, and keep track of what is happening. A good leader stays calm, listens to team members, and encourages clear communication. By staying organized and confident, they help the team work together smoothly and give the patient the best chance for a positive outcome.
1. Team Leader
Every resuscitation team needs a clear leader. The leader gives everyone their jobs, decides on treatments, and checks in with the team to make sure things are going smoothly. If a role is not filled, the leader steps in to handle it. By guiding the team and keeping everything on track, the leader helps the group work together and care for the patient effectively.
2. IV/IO/Medications
The IV (intravenous)/IO(intraosseous) and medications provider starts the IV or IO line and gives the needed medicines during a resuscitation. They work closely with the team to make sure treatments are given at the right time. By staying focused and organized, they help support the patient and keep the resuscitation running smoothly.
3. Timer/Recorder
The timer and recorder keep track of when treatments and medications happen and lets the team know when the next ones are due. They also note how often chest compressions are paused and for how long. By sharing this information with the team leader and everyone else, they help the group stay on schedule and make the resuscitation more effective.
Note: This is a suggested team formation. Roles may be adapted to local protocol.
8 Elements of Team Dynamics During Resuscitation
Resuscitation teams work best when everyone communicates clearly and supports each other with steady action. Strong teamwork boosts speed, accuracy, and confidence during critical moments.
1. Clear Roles and Responsibilities: In an ACLS high-performance team, everyone knows their job and what to do next. Clear roles help you stay calm, work smoothly, and act fast for the patient.
2. Knowing One’s Limitations: Everyone recognizes when they’re unsure or outmatched, and asks for help right away. This honesty keeps the team safe, speeds decisions, and protects the patient.
3. Clear Messages: Team members share concise, direct updates so everyone stays on the same page and acts quickly. Honest, simple communication helps prevent mistakes and keeps the patient the main focus.
4. Closed Loop Communication: This means repeating back instructions to make sure everyone is on the same page (platform).
For example,
- If a Team Leader Says: Give Two Breaths
- The Responder Replies: I Will Give Two Breaths and then complete the Task.
5. Knowledge Sharing: This helps everyone make better decisions during resuscitation. For example, a team member can quickly explain a patient’s history so the group knows the best next step.
6. Constructive Intervention: It means speaking up kindly when something could be done better. For example, if someone is compressing the chest too slowly, a teammate can say: Let’s speed up the compressions to keep the patient safe.
7. Mutual Respect: This means treating every team member’s ideas and actions as important. For example, listening carefully when a nurse suggests a change shows that everyone’s contribution matters.
8. Re-Evaluation and Summarizing: Regularly assessing patient status, treatment plan team performance, and summarizing key information to ensure everyone is on the same page.
Common Pitfalls in Team Performance
Resuscitation teams can struggle if roles aren’t clear, and if you miss quick updates or smooth handoffs. Let’s explore the common pitfalls of it.
- Role confusion can slow us down and blur who does what, so you should be clear about each person’s job from the start.
- Communication breakdowns happen when messages aren’t heard, so you need concise updates and readbacks to stay on the same page.
- Delayed interventions occur when priorities aren’t obvious, so you must agree on the highest focus and act quickly.
- Overcrowding at the patient’s side makes tasks harder, so you should keep only essential people nearby and rotate teammates as needed.
Training and Practice for High-Performance Teams
- You practice regular mock codes because they train you to react fast and stay calm.
- Your team gives feedback and debriefs after simulations and real events to help you improve.
- You build confidence through repetition so you can act with clarity during emergencies.
Post-Resuscitation Team Actions
- You give immediate post-ROSC care to stabilize the patient right away.
- Your team transfers the patient to the next level of care for ongoing support.
- You debrief together afterwards to find ways to improve for next time.
Key Takeaways for High-Performance Teams
In summary, a well-organized ACLS high-performance team depends on clear roles, steady communication, and quick, coordinated actions. When the compressor, AED/monitor operator, airway person, leader, IV/IO/medications provider, and timer work as one unit under strong leadership, the code runs more smoothly and safely. Everyone knows the plan, stays focused on the patient, and can adapt as conditions change, which means faster decisions and a better chance of recovery. With practice, feedback, and a calm, collaborative mindset, teams can turn tense moments into confident, life-saving care.
Get certified in a day with Same Day CPR. Our AHA ACLS, BLS, PALS, CPR, and First Aid programs start with an online course, followed by a concise 30-minute in-person skills session at a convenient center. Your official American Heart Association certification card is issued immediately. Visit our Locations or Classes page for details and registration.